
In some cases, the doctor will let the fluid drain through the tube for a few hours. You will be closely watched for several hours. Pressure is applied to the injection site for several minutes to stop any bleeding.Īfter the procedure, you will have a chest X-ray to check for possible puncture and collapse of your left lung. Or the tube may be left in for up to a few days. You must remain very still throughout the procedure.Īfter some or all of the fluid is drained, the tube may be removed right away. At different times during the procedure, you may be asked to hold your breath. Some fluid may be saved and sent to a lab for tests. The doctor may guide a thin plastic tube along the needle into the space between the sac and your heart. Or an X-ray camera may be used to guide it. Your doctor may use an echocardiogram to help guide the needle. The needle is then slowly pushed through the pericardial sac into the space between the sac and your heart. (In some cases, the needle is inserted between your ribs on the left side, over your heart.) Then a long, thin needle will be carefully inserted just below your breastbone. You will get a shot of anesthetic to numb your skin and deeper tissues. You may get a mild sedative to help you relax. The pressure from excess fluid can prevent normal filling of the heart, which can reduce the heart's ability to pump blood ( cardiac tamponade). This helps relieve pressure on the heart. Pericardiocentesis may also be done to treat pericardial effusion by removing the blood or excess pericardial fluid surrounding the heart. The fluid is sent to a lab where it is measured and checked for blood, microorganisms (such as bacteria, fungi, or viruses), white blood cells, sugar (glucose), cancer cells, and other substances. During this test, a needle is inserted into the chest and into the pericardium to remove a sample of the fluid. The test may be done to find the cause of a pericardial effusion. This fluid collection is called pericardial effusion. Some diseases cause fluid to collect within the pericardium. It helps reduce friction between the heart and other structures in the chest when the heart beats. This fluid surrounds and helps cushion the heart. Normally, there is a small amount of fluid between this sac and the heart. It protects the heart and parts of the major blood vessels connected to the heart. The tissue sac that surrounds the heart is called the pericardium. The outcome of treatment may depend on the cause and severity of the condition, how quickly treatment is started, and your overall health.Pericardiocentesis is done to find the cause of fluid buildup around the heart and to relieve pressure on the heart. Symptoms often improve greatly after the excess fluid is drained. 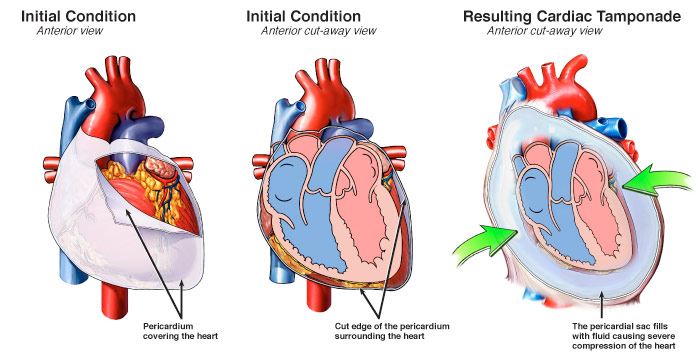
Your provider might be more likely to do this if you've had chronic pericardial effusion. It can also prevent the fluid from building up again. This is done to help diagnose the cause of the effusion. The surgeon may remove a piece of the pericardium. In some cases, the pericardial sac may be drained during surgery. This procedure uses a needle and a thin, flexible tube (catheter) to drain the fluid. The fluid is drained with a procedure called pericardiocentesis. Treatment of pain with aspirin or another medicineĪ severe pericardial effusion may need to be drained. Therapy aimed at the cause of the effusion, such as antibiotics for a bacterial infection or medicines, such as ibuprofen, for inflammation If a pericardial effusion is not severe, treatment may include:Ĭareful monitoring with repeated echocardiograms Chronic and acute pericardial effusions may require different treatment. It will also depend on how severe the condition is and what caused it. Treatment will depend on your symptoms, age, and general health. Chronic pericardial effusion occurs when cardiac effusion happens more than once over time. This is known as subacute pericardial effusion. This is known as acute pericardial effusion. In some cases, pericardial effusion develops quickly. 
But not all pericardial effusions cause cardiac tamponade. This can reduce the amount of oxygenated blood going out to the body. Because the heart can't expand normally, less blood can enter the heart from the body. This condition is called cardiac tamponade. But if too much fluid builds up, it can make it hard for the heart to expand normally. In some cases, extra fluid can build up between these two layers leading to a pericardial effusion.Ī little fluid won’t cause much of a problem. The fluid reduces friction between the two layers as they rub against each other during each heartbeat. Normally, there is a small amount of fluid between them. This can prevent it from pumping normally.Ī fibrous sac called the pericardium surrounds the heart. If too much fluid builds up, it can put pressure on the heart. Pericardial effusion is the buildup of extra fluid in the space around the heart.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
